
In rural America, alarm bells are sounding. Since 2010, more than 180 rural hospitals have quietly shut their doors or stopped offering inpatient care.
The latest data show nearly half of the remaining 900+ rural hospitals are operating at a loss, and 432 are considered “vulnerable” to closure. For the 46 million Americans living beyond city limits, shrinking local services risk turning their communities into healthcare deserts.
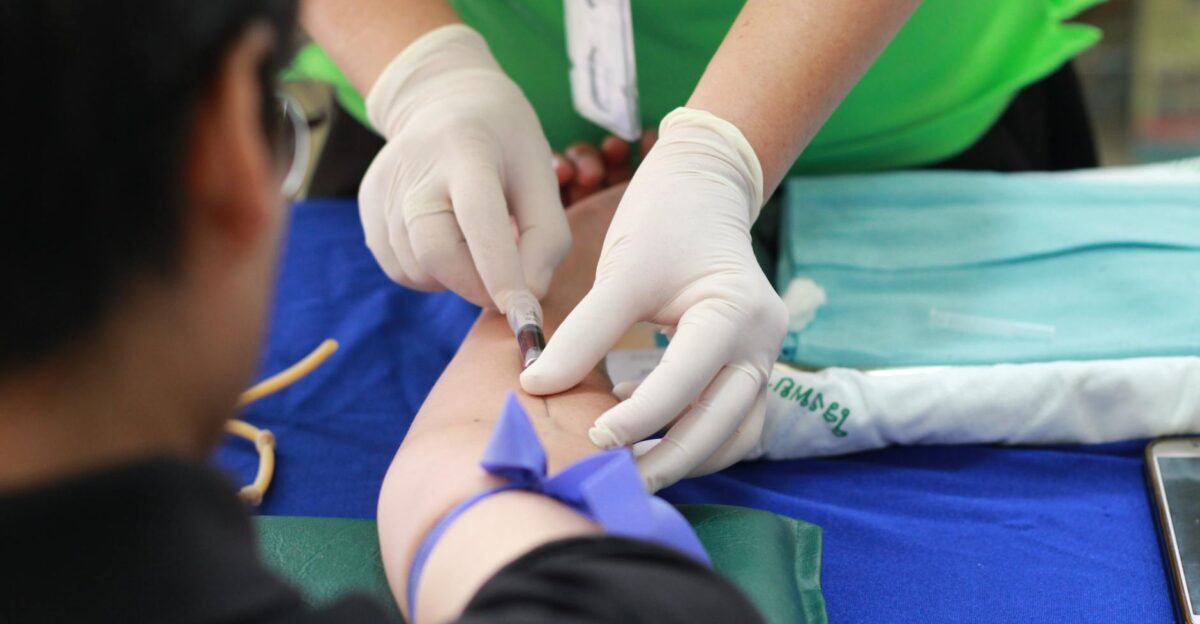
These problems emerge amid chronic doctor shortages and economic pressures, suggesting the rural safety net is at breaking point.
Accelerating Trend

Even as this crisis builds, the pace of closures is picking up. In the past few months alone, at least 13 rural clinics announced shutdowns across states like Virginia, Minnesota, and Maine.
This string of announcements – the fastest wave of rural consolidations in recent memory – has experts on edge. Many point to the looming $1 trillion cut in Medicaid funding starting in 2027 as the trigger. If that holds true, analysts warn this regional crisis could snowball nationwide within a year or two.
What’s happening in a handful of towns today could spread across the country by 2027.
Decades of Vulnerability

These closures didn’t come from nowhere. For over a decade, rural hospitals have labored under fragile finances. From 2010 to now, 182 rural hospitals have already closed or converted to outpatient-only models.
The communities they serve generally earn much less than city-dwellers and suffer higher rates of chronic illness. Nearly half of the remaining rural hospitals lose money every year.
Over the years, federal programs (like Medicaid reimbursements) have been a lifeline. Without them, many small hospitals wouldn’t survive. In short, rural healthcare has always walked a financial tightrope — now the rope is fraying.
Perfect Storm
Now those economic tightropes face a perfect storm. Healthcare costs have soared: inflation and sky-high staffing expenses (driven by contract labor and nursing shortages) are squeezing budgets.
At the same time, patient visits are flat or declining, so revenues fall. For example, Kansas – where 87% of hospitals already run in the red – has seen hospitals deferring maintenance and pay raises just to stay afloat.
Across rural America, experts say it feels “like a perfect storm” – rising costs and falling patients at once, leaving small hospitals with virtually no margin for error.
Legislative Impact
Then came the recent budget law, and with it, a major shock to rural clinics. The so-called “One Big Beautiful Bill Act,” signed July 4, 2025, makes deep cuts to Medicaid over the next decade. This provoked immediate dread among rural doctors and patients.
In Tennessee, retiree Lisa Parisot put it bluntly: Medicaid changes could be “a matter of life or death,” she warned. “I’m all for trimming the fat,” she added. “But it’s the people that are dramatically affected”.
Within days, Augusta Medical Group in Virginia cited the new law by name when it announced plans to consolidate three rural clinics.
Virginia’s Warning
Augusta Health’s actions in Shenandoah Valley highlight the stakes. Last month, the system officially closed Weyers Cave Urgent Care, Buena Vista Primary Care, and Churchville Primary Care.
Patients from those towns – each only served by a single small clinic – now must drive 8–10 miles further for basic care.
Augusta’s president, Kris Doan, said the consolidation was “necessary to ensure the future” of the system and noted it was tied to the budget law’s fallout. Virginia’s U.S. Senators Mark Warner and Tim Kaine echoed this as a warning shot.
Human Cost
Residents and families in these towns are already feeling the squeeze. Democratic strategist Marshall Cohen worries Virginia’s closures are only “the tip of the iceberg”.
Candice Crow, a mother of four children with autism who relies on Bon Secours – Southampton Medical Center in Franklin, Virginia, expressed concerns about access to care. “Every minute counts when it comes to emergencies. This could cost someone their life, so you’re taking away their lifeline.” —Candice Crow, Franklin, VA resident, as reported by CNN, Sep 22, 2025.
Rural communities disproportionately depend on Medicaid and safety-net clinics, so when one closes, thousands of poor or uninsured people face much longer drives for care. In practice, that means more cars on icy roads for an ER visit, and fewer routine checkups to catch illness early.
A Nationwide Pattern
Distressing as it is, the Virginia example is not unique. Across the map, communities report the same story. In Nebraska, Curtis Medical Center announced it will close by Sept. 30, explicitly blaming federal funding uncertainty.
Maine’s Central Maine Healthcare has said at least three of its rural clinics will close this month. And in Minnesota, the nonprofit Mayo Clinic recently disclosed plans to shut six rural primary care clinics by December.
(Mayo emphasizes this was for efficiency, not directly Medicaid cuts.) Notice something: these shutdowns are happening in Republican and Democratic states alike.
Economic Ripple Effect

This is more than a health issue – it’s an economic earthquake for small towns. Often, the local hospital is the biggest employer, supermarket, and lab. For example, the Curtis Medical Center (Neb.) has served Frontier County and even provided a student health clinic for the Nebraska College of Technical Agriculture for 30 years.
Its closing won’t just disrupt clinic hours – it will cost jobs and leave the nearest hospital tens of miles away. Economists note that when a rural hospital dies, local economies and mortality both suffer. (Research shows rural hospital closures have been linked to roughly a 6% rise in local mortality rates.)
Even beyond healthcare, shuttering these community anchors tends to trigger population decline, lost tax base, and businesses dying off. In short, one more hospital closed means many more families and farms left vulnerable.
Financial Mechanisms

It gets tricky behind the scenes, too. Federal changes will slash a crucial funding tool: provider taxes. Almost every state uses a tax on hospitals and insurance companies to pull down extra federal Medicaid dollars.
Under the new law, the allowable provider tax will fall from about 6% of revenue to 3.5% by 2034. That new cap will sweep away billions in matching funds: 48 states currently have taxes above 3.5%.
State governments then face hard choices. Do they raise other taxes, or simply pay doctors and hospitals less? Missouri Sen. Josh Hawley warned that the current plan is forcing rural hospitals to close to pay for tax cuts elsewhere: “It’s just not the right thing to do to shut down a bunch of rural hospitals to pay for tax cuts,” he said.
Industry Frustration

Hospital leaders are seething. Across the country, CEOs of community hospitals are publicly begging for help. “The current financial environment… has made it impossible for us to continue operating all of our services,” said Troy Bruntz, CEO of Community Hospital in McCook, Nebraska, explaining his pending clinic closure.
He’s not alone: similar stories are unfolding in Texas, Missouri, and Ohio. Executives note that even after years of belt-tightening – deferring maintenance and wage increases – they simply can’t absorb higher supply costs plus steep reimbursement cuts simultaneously.
Many say the government left them no path forward. Put another way, these administrators feel like they’ve been playing a rigged game – and now all the chips are falling out of the rural healthcare economy.
Strategic Consolidation
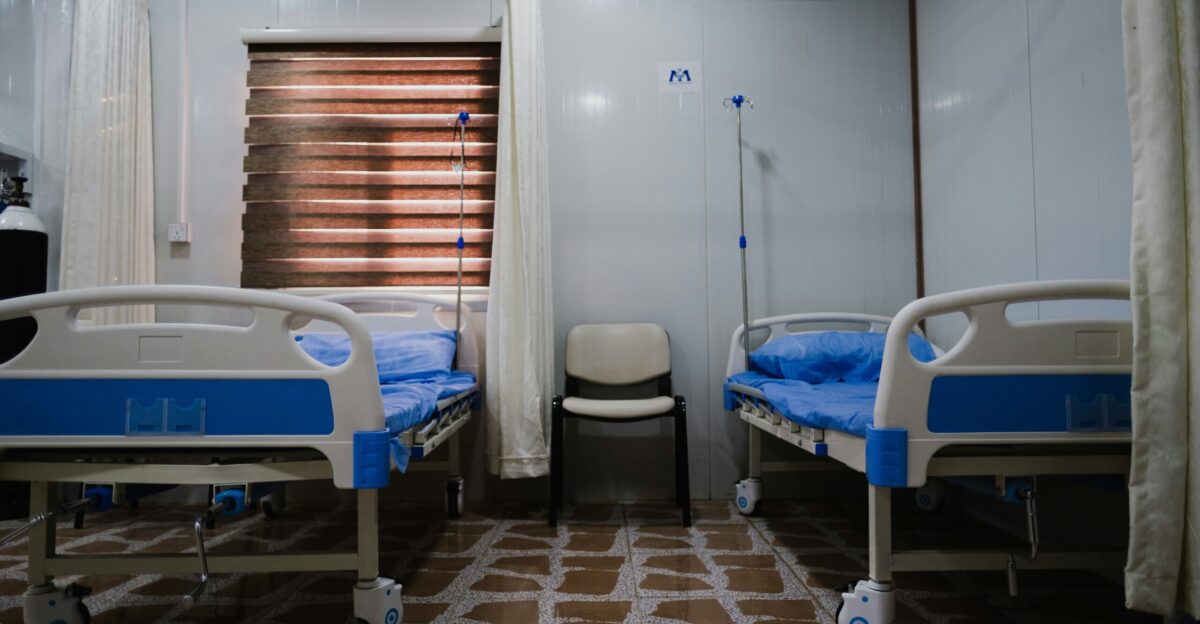
Meanwhile, large health systems cast their moves differently. Mayo Clinic, for instance, calls its Minnesota shutdowns “consolidation” and modernization. In public statements, Mayo stressed it will move care into centers “with infrastructure, staff, and support in place” to serve rural patients.
In their words, they’re simply adapting to tougher economics. But critics question that narrative. Brad Arends, president of the Albert Lea Healthcare Coalition, points out the irony: Mayo rakes in hundreds of millions in revenue each year, yet “says they can’t afford to provide health care to towns the size of Albert Lea”.
Town officials and civic groups are fuming that a nonprofit giant can cut off small communities while keeping big-city earnings. These debates — about profit vs. community service — are opening a fresh front in the rural crisis.
Recovery Efforts

In Congress, some Republicans insisted on a safety net for rural areas. The final budget deal includes a new Rural Health Transformation Program: $50 billion total, $10 billion per year over 5 years, for states to shore up rural providers.
GOP leaders call it historic – Sen. Mike Crapo (R-ID) touted it as “the single largest investment in rural health care since 2003”.
Practically, states now have until Nov. 5, 2025, to apply for this funding; CMS plans to award grants by Dec. 31, 2025. Ideally, this fund could help buy new equipment, build telehealth networks, or cover lost revenue.
Expert Skepticism

Public health analysts are skeptical. Many call the $50B fund a drop in the bucket compared to the cuts coming. By one estimate, Medicaid reductions will cut rural spending by about $137 billion over 10 years – roughly 2.5 times the new fund’s size.
KFF’s Zachary Levinson warned lawmakers that even if all the $50B materializes, “it’s unclear what portion…would eventually go to hospitals” versus other uses.
the funding could be diluted into pilot projects or broadband grants, rather than direct support to crisis facilities. Bottom line: Experts say that unless the program is targeted carefully, $50B may not forestall the worst damage. It might stabilize some hospitals, but many fear it won’t be enough to offset the sheer scale of cuts ahead.
Future Implications

Sadly, the worst may still lie ahead. Most new Medicaid cuts don’t kick in until 2027, so many communities haven’t yet felt the full impact. Officials predict the current closures may be just the beginning.
In Nebraska, health leaders say six hospitals are already “critical” and could go under “within a year or two” after cuts fully hit.
Nationally, an analysis by UNC’s Sheps Center suggests about 338 rural hospitals are so financially distressed they face closure unless help arrives. Put simply, for tens of millions of rural Americans, local ERs and clinics could vanish almost imperceptibly — making it hard for policymakers and families to comprehend how bad things have gotten until it’s too late.
Political Battleground

This unfolding crisis is rapidly becoming a political flashpoint. Rural healthcare will be a key battleground in the 2026 midterms. Democrats already highlight each clinic closing as proof of GOP policy failures.
In Virginia, both parties have staked out burned-out towns in campaign ads. National Democrats even coined a nickname for the budget law: “One Big, Ugly Bill.” House Minority Leader Hakeem Jeffries posted on social media that it is “devastating rural hospitals in Virginia and across the nation”.
Republicans counter that they did invest like never before, pointing to the $50B fund as “historic.” But on the ground, voters are unsettled by rising health costs and shrinking access.
State-Level Responses

Already, state governments are reacting in different ways. Some are taking pre-emptive budget measures. For example, North Carolina and Idaho this summer announced cuts to Medicaid provider payments to hospitals and doctors, even before the federal law fully applied.
Other states are revising or dropping so-called “provider taxes” that no longer qualify for matching funds.
The patchwork is growing: two neighboring rural counties might have very different care access depending on their state’s policy mix. Analysts warn this could reshape the US medical map, as rural patients migrate toward any safe pockets of care.
Legal and Regulatory Pressure

On top of politics, there are legal and regulatory headaches. Some state attorneys general have hinted at lawsuits to block parts of the federal changes, though Virginia’s AG so far has not joined any multistate action.
Meanwhile, rolling out work requirements, eligibility checks, and new tax rules all at once is a massive undertaking. Many state Medicaid agencies are stretched to implement changes on deadline.
We may see federal judges drawn in to sort out eligibility rules and funding disputes. In practice, this swirl of lawsuits and regulations adds uncertainty, possibly delaying relief to hospitals already counting the days until they run out of cash.
Cultural Transformation

With the old safety net fraying, rural healthcare delivery is evolving by necessity. Telemedicine networks are expanding rapidly to reach patients at home. Major systems are deploying mobile clinics (Augusta Health just christened a state-of-the-art mobile unit this summer, to bring wellness visits and chronic care directly into neighborhoods).
Some communities are forming their own solutions. In Albert Lea, MN, local donors and businesses raised millions to lease clinic space, even hiring two retired Mayo doctors part-time to staff it.
These adaptations – telehealth, mobile vans, health co-ops – could make rural care more flexible. But experts caution: such stopgap fixes may improve access, but they usually can’t fully replace full-service hospitals.
Defining Moment

Ultimately, the turmoil in rural healthcare represents a defining test of national priorities. As urban medical centers consolidate and innovate, rural regions risk becoming true “healthcare deserts” where even emergencies require long travel.
Chartis researchers put it plainly: for rural Americans, “the rapid deterioration of access to care…raises pointed questions about the safety net’s ability to continue to meet the needs of these communities”.
The National Rural Health Association notes over 180 rural hospitals have already closed since 2010 and roughly half of the rest are loss-making. Over the next two years, we’ll see whether Congress and communities can fortify care with innovative funding and delivery—or watch entire regions go without basic medical services.